How rising Medicare premiums could impact your 2026 Social Security check
The financial landscape for millions of American seniors is set to shift significantly in 2026, as a substantial increase in Medicare Part B premiums is poised to consume a considerable portion of their anticipated Social Security cost-of-living adjustment (COLA). For the first time, the monthly charge for Medicare Part B will surpass the $200 mark, an increase that threatens to erode the purchasing power of seniors who rely heavily on their Social Security benefits.
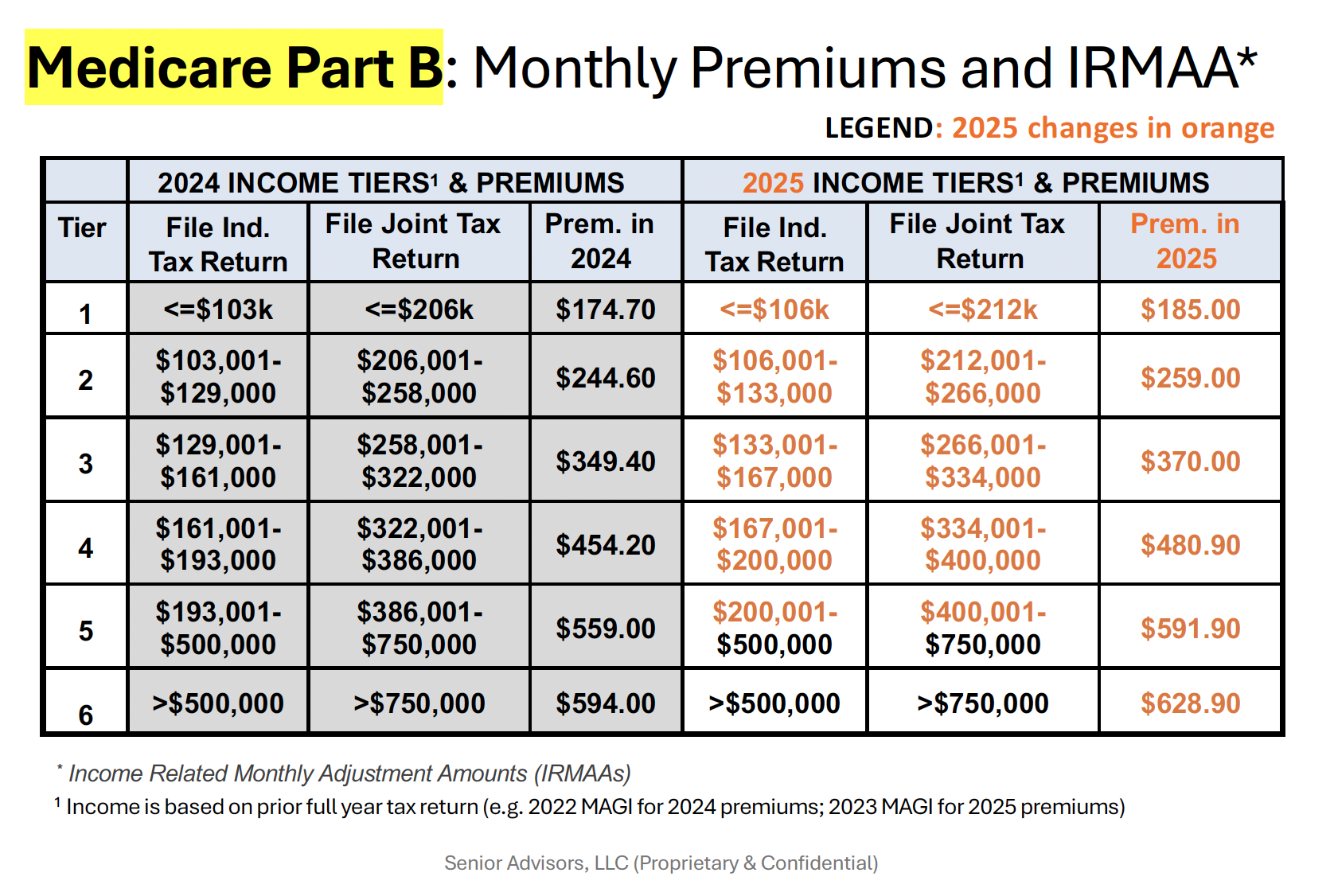
Earlier this month, the Centers for Medicare & Medicaid Services (CMS) announced that the premium for Medicare’s Part B, which is vital for covering doctor visits, outpatient care, preventive services, and other essential medical services, will jump by 9.7%. This translates to an increase of $17.90, pushing the monthly cost from the current $185 to $202.90. This significant hike marks the largest increase since 2022, when beneficiaries saw a 15% surge in their Part B premiums. Beyond the monthly premium, the Part B deductible – the out-of-pocket amount seniors must pay before their coverage begins – is also slated for a roughly 10% increase, climbing from $257 to $283 next year.

These Medicare Part B premiums are automatically deducted from beneficiaries’ monthly Social Security checks, meaning that the increase will directly impact the net amount seniors receive. This direct link makes the premium hike a critical concern, especially for those on fixed incomes. According to Anne Montgomery, a senior health policy expert at the National Committee to Preserve Social Security and Medicare (NCPSSM), the premium is rising at a rate approximately three times that of inflation. This disparity is primarily attributed to a broader rise in underlying healthcare costs and increased demand for medical services. Max Richtman, the president and CEO of NCPSSM, underscored the gravity of the situation, telling CBS News, "So many rely on [Social Security] for all or most of their income. This is gonna hurt."
The Social Security Administration has determined next year’s cost-of-living increase at 2.8%, a figure designed to help benefits keep pace with inflation. This adjustment is projected to boost the average Social Security paycheck by $56, bringing the monthly average to approximately $2,071. However, the substantial Medicare Part B premium hike is expected to consume roughly one-third of this COLA. NCPSSM’s analysis suggests that this effectively lowers the actual purchasing power of the COLA to about 1.9%, a figure significantly below the current inflation rate of 3%. For seniors with lower monthly benefits, the impact could be even more severe, potentially resulting in an effective COLA of zero, leaving them with no additional funds to cope with other rising living expenses.
The primary drivers behind these escalating costs are multifaceted, reflecting systemic challenges within the U.S. healthcare system. General healthcare inflation, influenced by everything from labor costs for medical professionals to the price of medical supplies, is a consistent factor. Beyond this, CMS points to increased demand for medical services as a key contributor. As the baby boomer generation continues to age, the sheer volume of individuals entering Medicare and requiring more intensive medical care naturally increases utilization and, subsequently, costs.
Moreover, the rising cost of prescription drugs, especially new specialty medications for chronic conditions like cancer, diabetes, and autoimmune diseases, plays a substantial role. While offering life-changing treatments, these innovations often come with a hefty price tag that trickles down to affect overall Medicare expenditures. Similarly, advancements in medical technology and diagnostic tools, while beneficial for patient outcomes, contribute to higher treatment costs. The labyrinthine structure of the U.S. healthcare system itself, with its complex billing, insurance, and administrative processes, also contributes to higher overhead costs compared to other developed nations. In 2023, Americans spent an average of $1,514 on out-of-pocket healthcare costs, representing a 9% increase from 2020 on an inflation-adjusted basis, illustrating the growing financial burden on individuals across all age groups.
The burden of rising healthcare premiums isn’t confined solely to Medicare beneficiaries. Working adults are also facing similar pressures. Approximately 22 million Americans who obtain their health insurance through the Affordable Care Act (ACA) marketplaces are bracing for steep rate hikes in 2026. This looming crisis stems from the potential expiration of crucial premium tax credits, which are set to lapse at the end of 2025. These credits are instrumental in lowering the cost of coverage for the vast majority of people enrolled in ACA plans. The extension of these tax credits became a major point of contention in recent government shutdown debates. Without legislative action to extend them, KFF estimates that Americans relying on these tax credits could see their healthcare costs more than double in 2026, leading to widespread "sticker shock." Similarly, workers covered by employer-sponsored health plans are also likely to see their costs climb next year, with analyses from consultants like Mercer projecting that most will pay 6% to 7% more for their 2026 plans.
For seniors, the implications of these rising costs are particularly stark. Many live on fixed incomes, making any reduction in their net Social Security benefit a significant hardship. The effective erosion of their COLA means less money available for essential expenses such as food, housing, utilities, and transportation, potentially forcing difficult choices between healthcare and other necessities. Advocacy groups like NCPSSM continue to highlight these challenges, urging policymakers to consider comprehensive solutions to safeguard the financial well-being of older Americans.
Seniors are not entirely without recourse in navigating these increases. It is crucial for beneficiaries to review their Medicare plans annually during the open enrollment period to ensure they have the most cost-effective coverage for their needs. This might involve comparing Original Medicare with a Medigap policy to Medicare Advantage (Part C) plans, which often have different premium structures and out-of-pocket limits. Additionally, individuals with lower incomes may qualify for Medicare Savings Programs (MSPs) or the Low-Income Subsidy (LIS) for Part D prescription drug costs, which can help cover some or all of their premiums and deductibles. Financial planning and careful budgeting will also become increasingly vital for managing healthcare expenses alongside other living costs.
The confluence of rising healthcare expenditures and the mechanisms for funding Medicare necessitates a critical re-evaluation of policy. As Medicare Part B premiums surge past $200 for the first time, threatening to significantly diminish the value of Social Security’s COLA, the call for sustainable and affordable healthcare solutions for seniors grows louder. The financial security of millions depends on addressing these systemic issues head-on, ensuring that vital benefits remain adequate to meet the escalating costs of living and healthcare.